Ha-Joon Chang in �23 Things They Don�t Tell You About Capitalism� argues �equality of opportunity is not enough. Unless we create an environment where everyone is guaranteed some minimum capabilities through some guarantee of minimum income, education, and healthcare, we cannot say that we have fair competition. When some people have to run a 100-metre race with sandbags on their legs, the fact that no one is allowed to have a head start does not make the race fair. Equality of opportunity is absolutely necessary but not sufficient in building a genuinely fair and efficient society.�
Even as the world goes through the third wave of this COVID-19 pandemic, driven mainly by the delta variant of the SAR-Cov-2 virus, data from Public Health England gives the clearest indication that the link between infection, hospitalisation and death has been partially broken. Though the number of new cases in the United Kingdom have been going up and have reached daily numbers not seen since February of this year, the hospitalisation and mortalities numbers have not matched up.
For example, in the week ending 2nd of February, the 7-day average number of mortalities were 1,122 (7-day average daily new cases 23,268) compare with 18 deaths for the week ending 2nd of July (7-day average daily new cases 22,186). The 98.4% drop in mortality has been attributed to the role vaccination has played in protecting the most vulnerable in the population. The current uptick is concentrated in the segment of the population yet to be vaccinated. It further indicates that all three vaccines being used in the UK (Pfizer, AstraZeneca and Moderna) are highly effective in ensuring that economic activity can return to a semblance of normalcy.
Unfortunately, this level of population protection has not been provided evenly globally. A look at the data on Global vaccination coverage indicates that out of the approximately 3.5 billion vaccine doses that have been administered, 50.4% have been used in Asia, 21.54% in North America, 19.77% in Europe, 6.4% in South America, 1.62% in Africa and 0.26% in Oceania. The African Centre for Disease Control indicates that only 1.1% of the 1.3 billion people in Africa have been fully vaccinated. This is up from 0.98% a couple of weeks ago., a very slow creep.
This must be a matter of concern as genomic sequencing across the continent suggest that the current wave of the pandemic is being driven by the delta strain. This variant with a reproductive number between 5 and 8, if left unchecked, could soon overburden the continent�s health systems. As if this was not bad enough, it has now emerged that the European Union (EU) is failing to recognize the batch numbers of the version of the Oxford-AstraZeneca vaccine manufactured by the Serum Institute of India (SII).
Initially, the impression was created that this non-recognition by the EU was due to the vaccines manufactured by SII being of inferior quality. We want to emphasise that this is not the case.
Based on the batch manufacture data available for Vaxzevira (the version of the vaccine available in the EU) and Covishield (the version manufactured by SII), there is no doubt that they are equivalent. Currently, five million doses of the SII version have been administered in the UK. The issue at play is more to do with registration technicality and patent economics. The EU is taking a position that Covishield has not applied for and obtained Emergency Use Authorisation (EUA) from the European Medicines Agency (EMA). Thus, their batch numbers cannot be coded as part of the bloc�s digital travel certificate that will exempt fully vaccinated travellers from entering their jurisdiction without undergoing the certified period of quarantine.
This situation, if not rectified, will affect not just African citizens majority of whom have received doses of the AstraZeneca vaccine, but many countries that are part of the COVAX platform. As at the time of writing, we were aware that the EU had alluded to the fact that individual countries could opt out of this administrative decision; a further confirmation that the effectiveness of this version of the vaccine is not in doubt. However, this exemption only applies to vaccines on the World Health Organisation (WHO) COVID-19 EUA list. The result is that nine EU countries (Austria, Germany, Greece, Slovenia, Iceland, Ireland, Estonia, Spain and Switzerland) have indicated that they will allow fully vaccinated people travel access without mandatory quarantine in line with the prevailing public health advice.
It is easy to fault the EU for dealing Africans with a raw card without considering the intellectual property and economic implications of this tussle. However, it is important to understand that there is merit in their approach. When any new medicine is approved by any regulator, there is a period within which that medicine is within the patent. This provision is to ensure that developers can benefit from their innovations. Until this period has elapsed, global pharmaceutical licensure agreements prohibit the manufacture of the said medicine out of patent. This provision was a barrier during the HIV/AIDS pandemic and resulted in India violating global patent laws to manufacture generic copies of antiretroviral medicines. Apart from this leading to a drop in the prices of these medicines on the pharmaceutical market, and better management of HIV in many countries, it led to a global feud followed by discussions on the prudence of patents during a global pandemic.
The result was that pharmaceutical companies and governments that invest heavily in medicines research and development accepted that under certain circumstances, patent restrictions could be lifted when global public health was threatened. It is not beyond doubt that with the WHO declaring COVID-19 a Public Health Emergency of International Concern (PHEIC), the patent restrictions could be eased. However, at the recent G-7 summit in the UK, leaders could not agree that patent rights on COVID-19 vaccines should be lifted. This was because of the huge investment biotechnological companies such as BioNTech SE, Novavax and Moderna had made during the R&D stages of vaccine development.
Unlike Oxford whose R&D was funded mainly by the UK taxpayer, these companies have shareholders who expect returns from the sale of these novel vaccines. Therefore, their governments have an interest in protecting the investments of the citizens and the longevity of these companies, and therefore were opposed to the lifting of patent rights. On the contrary, the UK government, as part of their COVID-19 strategy, anticipated this hurdle and opted to fund the design of vaccines that were cheap at the point of sale, with favourable cold chain requirements and were prepared to encourage AstraZeneca to enter into bilateral agreements for manufacture of their vaccines. This strategy accounts for the huge price disparity between the AstraZeneca vaccine ($3-$4 per dose) and all other vaccines currently on sale (lowest price $10 per dose).
We hope that whilst the WHO and the UK government work to find a lasting solution with the EU, African countries will put their house in order and digitalise their COVID vaccine travel certificates in anticipation of a favourable outcome. Last we checked, the QR code provided to fully vaccinated Ghanaians was dysfunctional and not activated. In other African countries, it is known that a digital certificate for fully vaccinated people is non-existent and not on the cards. This will not suffice as due to forgery, no country will accept paper handwritten documents as evidence.
There is enough data from the forgery of PCR certificates required for travel, to make it unwise for manual certificates to be allowed. Humans have become so deviant that despite the rapid appearance of variants of concern, some will be prepared to travel whilst not fully vaccinated. If this is allowed to occur, the global exit plan from this pandemic could be hampered. In the end, we believe a middle ground will be found that will allow free travel whilst protecting the patent rights of pharmaceutical companies. If these are not protected, the motivation to fund R&D will diminish and African countries will continue to show complacency when it comes to funding medical research. The point is, equality of opportunity must be promoted. It must also come with the willingness of the less resourced to contribute their quota towards global health security. Even though this can be said to be a matter of geopolitics and bureaucracy, the current vaccine travel certificate rumpus raises serious issues about the preparedness of Africa to raise its game in this area of health. Once again, we are bystanders at the table of health.
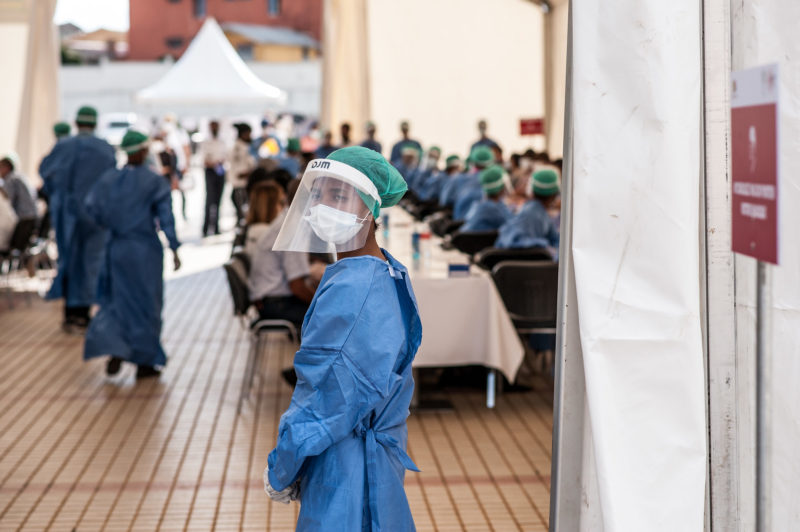 The Unseen Hand of Africa's Silent COVID-19 Community Spread
The Unseen Hand of Africa's Silent COVID-19 Community Spread
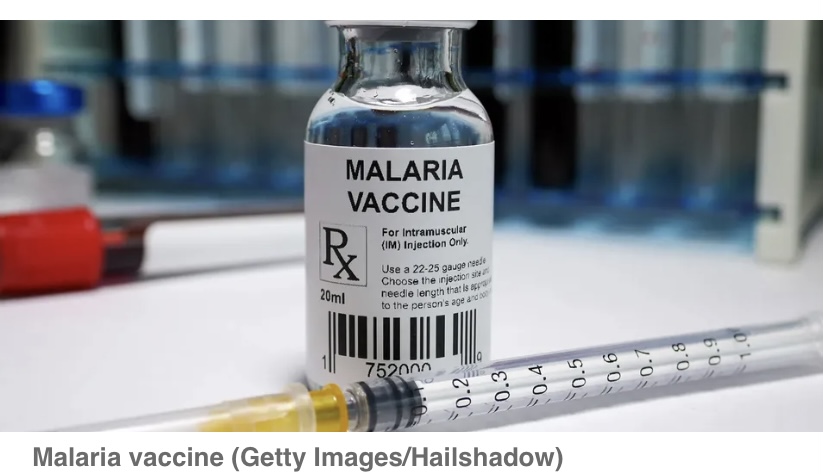 Vaccine Available: What Next for Africa's Fight Against Malaria?
Vaccine Available: What Next for Africa's Fight Against Malaria?
 Resolving the Challenges Around Vaccination Status Authentication
Resolving the Challenges Around Vaccination Status Authentication
 Pharmacy in Ghana: Evolving Towards Universal Health Coverage
Pharmacy in Ghana: Evolving Towards Universal Health Coverage
 Political Gaslighting Around Health Human Resource Recruitment
Political Gaslighting Around Health Human Resource Recruitment
 Unpacking the Confusion Surrounding the Testing Outcomes at KIA
Unpacking the Confusion Surrounding the Testing Outcomes at KIA
 Controlling Africa's COVID-19 Third Wave
Controlling Africa's COVID-19 Third Wave
 Confronting the Alarming Trend of Youth Suicide
Confronting the Alarming Trend of Youth Suicide
 Prioritising the Health of the African Citizen
Prioritising the Health of the African Citizen
 An Open Letter to President Akufo-Addo on Vaccine Geopolitics
An Open Letter to President Akufo-Addo on Vaccine Geopolitics
 Will Africa's Replacement Fertility Trends be a Blessing?
Will Africa's Replacement Fertility Trends be a Blessing?
 Factionalism and Feuding Risking Patient Safety in Ghana's Health System
Factionalism and Feuding Risking Patient Safety in Ghana's Health System
Copyright ©2021 MedicALL. Powered By Mojave